Credentialing Services
Professional Medical Provider Credentialing & Enrollment
At ONEX OMS LLC, we provide comprehensive Credentialing Services to help healthcare providers get approved by insurance payers quickly and accurately. Our credentialing experts manage every step of the process from application preparation to payer follow-ups, so you can focus fully on patient care.
We handle all credentialing requirements, payer contracts, re-credentialing deadlines, and enrollment updates with precision and compliance.
Complete Credentialing Support
We manage credentialing with Medicare, Medicaid, and major commercial payers, handling applications, submissions, and follow-ups for smooth approvals.
Faster Provider Enrollment
Our structured process speeds up approvals by tracking applications closely and resolving payer requests without delays.
Compliance & Documentation Accuracy
We ensure accurate, complete applications that meet payer guidelines, reducing errors and preventing unnecessary rejections.
ONEX OMS LLC Handles Your Credentialing Seamlessly
Credentialing is essential for providers to receive reimbursement, expand their patient base, and maintain payer relationships. At ONEX OMS LLC, we take the complexity out of credentialing by managing the entire process on your behalf.
Our services ensure:
✔ Complete and accurate credentialing applications
✔ Timely submission to all payer portals
✔ Follow-up with insurance companies
✔ Tracking of application progress
✔ Maintenance of compliance & renewals
We work closely with your office to collect all supporting documents and maintain accurate provider records — leading to smoother approval and fewer requests for missing information.

Our Core Credentialing Services
We offer end-to-end credentialing solutions that help providers get approved and stay active with insurance payers with minimal administrative burden.
Initial Credentialing Setup
Complete setup and preparation of profile, documents, and application packages.
Multi-Payer Enrollment
Enrollment with Medicare, Medicaid, and all major commercial insurers.
How Our Credentialing Process Works
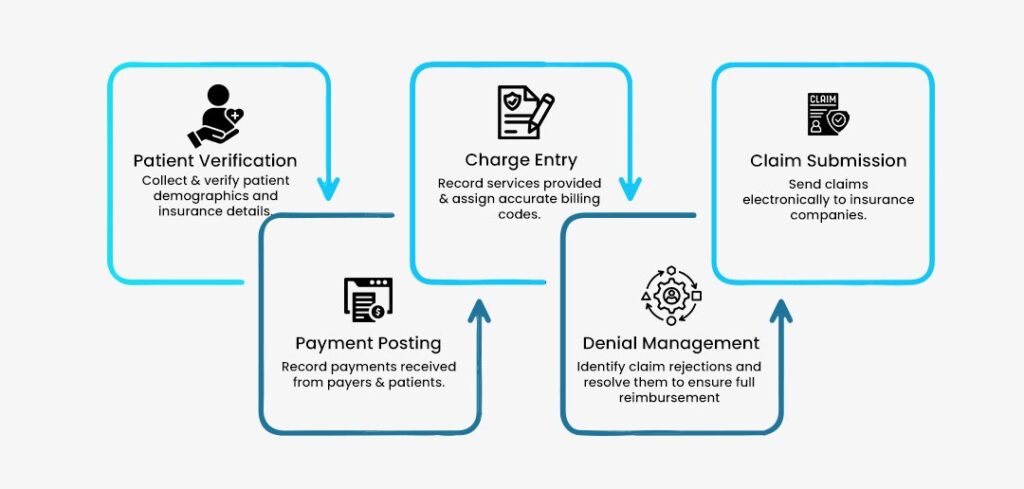
Reducing Credentialing Stress, Delays, & Revenue Gaps
Missing documentation, payer errors, or slow processing can delay approvals — and delay revenue. Our credentialing team minimizes administrative burden while keeping the process moving forward. With ONEX OMS LLC handling paperwork and payer follow-ups, approvals happen faster and with fewer obstacles.
Complete Credentialing Documentation
- License verification
- DEA / CDS certification
- Board certifications
- Practice details
Medicare Enrollment
- Application preparation
- Submission & tracking
- Timely updates
- Approval confirmation
Medicaid Enrollment
- State-specific enrollment
- Document compliance
- Follow-up management
- Status verification

Commercial Payer Credentialing
- Aetna, UnitedHealthcare, Cigna, Humana
- Anthem and Blue Cross plans
- Multi-network enrollment
- Contract verification
Re-Credentialing & Maintenance
- Expiration tracking
- Timely renewal submissions
- Provider updates
- Record accuracy
Provider Contract Support
- Contract review assistance
- Reimbursement term checks
- Payer notifications
- Credentialing status reports
Why Choose ONEX OMS LLC for Credentialing Services?
Expert Enrollment Specialists
Our team knows payer requirements and keeps every credentialing profile accurate and complete.
Faster Turnaround & Fewer Delays
We reduce administrative back-and-forth with payers, leading to quicker approval times.
Reduced Rejection Risk
Accurate applications and compliance review lower chances of rejections and repeat submissions.
Multi-Payer Experience
We manage credentialing across Medicare, Medicaid, and all major commercial plans.
Proactive Renewal Management
We track renewals and timelines so you never lose active status.
Streamlined Communication
We coordinate with your office and payers to keep you informed and prepared at every step.

Ready to Get Credentialed with Insurance Payers?
Let ONEX OMS LLC manage your credentialing process with accuracy and speed. Avoid paperwork stress and focus on patient care while we handle the rest.
