Insurance Eligibility Verification
Accurate & Timely Insurance Eligibility Verification Services
At ONEX OMS LLC, we provide comprehensive Insurance Eligibility Verification Services to ensure every patient’s coverage details are confirmed before services are rendered. Accurate verification helps prevent claim denials, reduce billing errors, and improve overall revenue cycle efficiency.
Our team verifies insurance coverage, benefits, copays, deductibles, and authorization requirements to ensure smooth claim processing and faster reimbursements.
Real-Time Coverage Verification
We verify patient insurance details before appointments to confirm active coverage and benefit eligibility.
Benefit & Authorization Checks
Our team confirms copays, deductibles, coinsurance, and prior authorization requirements to prevent billing delays.
Reduced Claim Denials
Accurate eligibility verification significantly lowers front-end errors and minimizes claim rejections.
ONEX OMS LLC Ensures Accurate Insurance Verification
Insurance verification is the first and most critical step in the revenue cycle. At ONEX OMS LLC, we ensure that all patient insurance information is thoroughly verified prior to service delivery.
We carefully review:
✔ Active policy status
✔ Coverage limitations and exclusions
✔ Copay, deductible, and coinsurance details
✔ Referral and authorization requirements
✔ Coordination of benefits (COB)
By identifying issues at the front end, we help practices avoid costly denials and ensure a smoother billing process.

Our Core Insurance Eligibility Services
We provide structured and accurate verification processes that improve claim acceptance rates and enhance patient billing transparency.
Pre-Appointment Verification
Insurance details are verified before the patient visit to avoid last-minute complications.
Authorization & Referral Management
We confirm whether prior authorization or referrals are required and ensure documentation is in place.
Step-by-Step Verification Process
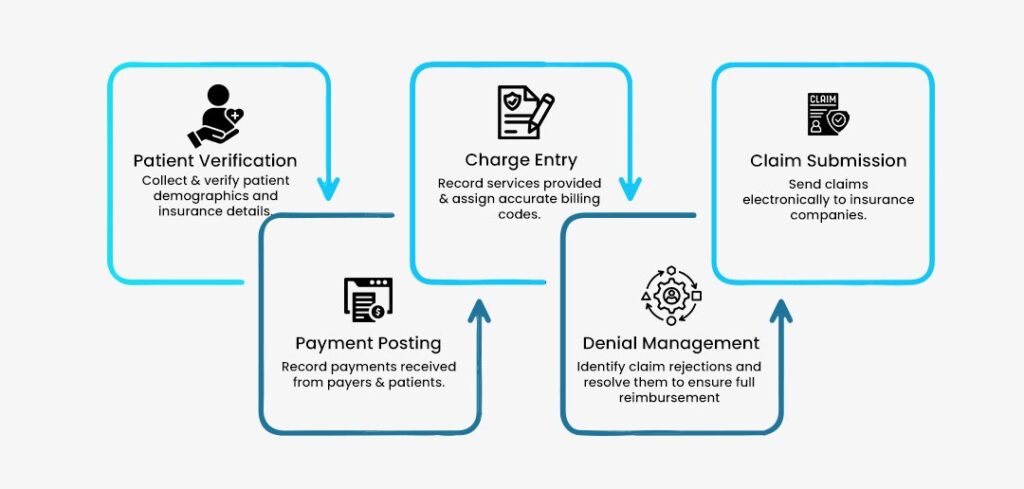
Strengthening Your Revenue Cycle from the Front End
Accurate insurance eligibility verification reduces claim denials, improves patient satisfaction, and ensures faster reimbursement. By confirming coverage before services are provided, we help practices avoid unexpected payment issues and revenue disruptions.
Active Coverage Verification
- Policy status confirmation
- Effective & termination date review
- Coverage type identification
- Payer validation
Benefits Investigation
- Copay verification
- Deductible status check
- Coinsurance details
- Out-of-pocket maximum review
Prior Authorization Review
- Procedure authorization check
- Referral requirements
- Pre-certification confirmation
- Documentation tracking

Coordination of Benefits (COB)
- Primary & secondary insurance review
- Correct payer sequence confirmation
- Avoid duplicate billing issues
- Accurate claim routing
Financial Responsibility Estimation
- Patient balance estimation
- Cost-sharing transparency
- Billing clarity
- Improved patient communication
Error Prevention & Compliance
- Front-end error reduction
- Clean claim improvement
- Documentation accuracy
- Payer guideline compliance
- Personalized support for every specialty practice
Why Choose ONEX OMS LLC for Insurance Eligibility Verification?
Improved Clean Claim Rate
Accurate front-end verification reduces billing errors and increases first-pass claim acceptance.
Reduced Claim Denials
By identifying coverage issues early, we minimize preventable rejections.
Faster Reimbursements
Verified claims move smoothly through the billing process, accelerating payments.
Experienced Verification Specialists
Our team understands payer policies and insurance guidelines across multiple specialties.
Better Patient Experience
Clear benefit verification prevents billing surprises and improves patient satisfaction.
Enhanced Revenue Stability
Strong front-end processes protect your practice from revenue loss and cash flow disruptions.

Avoid Claim Denials Before They Happen
Don’t let insurance errors delay your payments. Partner with ONEX OMS LLC to ensure accurate eligibility verification and smoother revenue cycle management.
